Florida has reopened for business for four weeks now and its experience is similar to that encountered by other states and countries that are trying to reopen quickly after COVID-19 lockdowns. Reopening the state for business is necessary and should be possible if enough testing and contact tracing resources are made available. However, testing capacity has always been surprisingly problematic for the US since January 11th when the genetic code for the novel coronavirus was first published and major countries such as South Korea and Germany were able to produce valid tests in quantity. To date, Florida and the US as a whole still lags behind South Korea, Germany, Taiwan, Australia, and other best-in-class countries in terms of testing completeness and thoroughness.
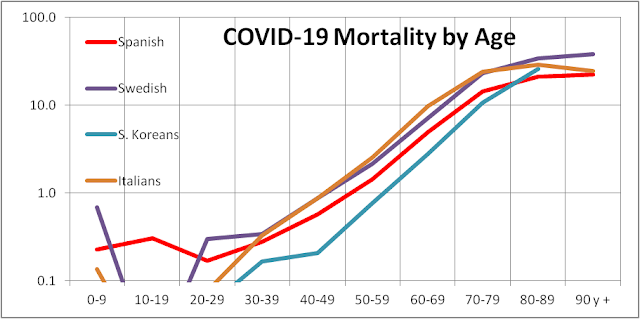
The figure below shows that testing (brown square against left axis) in Florida has expanded in two months from 6,000 per day in late March to near 24,000 per day now. The percentage of test results returning positive (blue diamond against right axis) has dropped from near 12% to near 3% now. All this is very encouraging although the unevenness of the recent data is worrisome especially in light of the recent complaints that (1) the data scientist compiling these data had been summarily dismissed, (2) thousands of tests have been invalidated because of poor handling, and (3) the count of virus tests and serological tests have been mixed inappropriately. Moreover, the improvement in testing completeness, after briefly touching 1% has now settled around 3.5% — suggesting that the overall Florida population may still be highly infected.
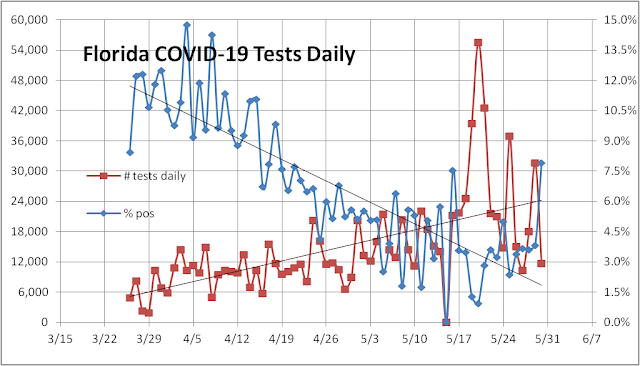
Another way to check progress in the War against COVID-19 is to look at the trends in daily confirmed cases in Florida. The figure below shows that in the month of April from roughly the time that the governor declared a state-wide lockdown to begin on April 2nd to the time when he began Phase 1 of reopening Florida on May 4th, the number of daily cases decreased steadily. So Florida’s lockdown did work to limit the number of cases and deaths in Florida. However, since the state began to reopen, the number of cases has begun to increase again in May. Some of this increase may be due to increased testing of asymptomatic and mildly symptomatic cases. But the recent leveling off in death count at 31 per day and the case fatality rate at 4.4% is worrisome. If you prefer to check progress via the effective reproduction number, R = 1.03, for Florida right now – borderline problematic in terms of renewed infection risk.
With Universal Studios set to reopen on June 5th and Disney World scheduled to reopen on July 11th, we are especially worried that South American tourists and snow birders entering their winter will be highly tempted to visit Florida. Thus far only travel from Brazil has been restricted but all of South America is severely infected and travel from there to the USA should be restricted for the next couple of months.