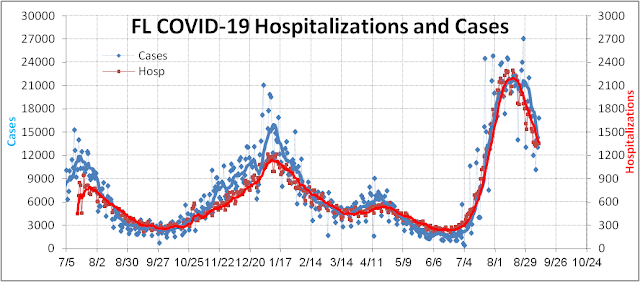
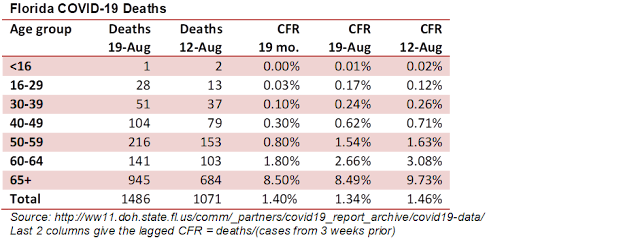
The COVID-19 pandemic had been relatively mild for children in 2020. In the early days, schools were shut and kids were sent home to learn remotely. Later when people found out kids were not as susceptible to serious illness from SARS-CoV-2, schools reopened and in-person learning was slowly restored with strong mitigation measures instituted. Pediatric hospitalizations (red curve in the figure below) increased last Fall but not too badly –running near 1.2% of adult hospitalization at the peak around the New Year. Late Spring 2021 with Delta edging onto the scene it became obvious that kids were more susceptible to this more contagious and possibly more virulent variant. Epidemiologists warned that school reopening without strong mitigation measures could lead to disaster and yet ironically more governors and parents went the opposite direction and eased mitigations. The end result is that pediatric hospitals were swamped and more kids suffered needlessly with MIS-C and other long COVID illnesses as pediatric hospitalizations are now at record levels = 2.4% adult hospitalizations.
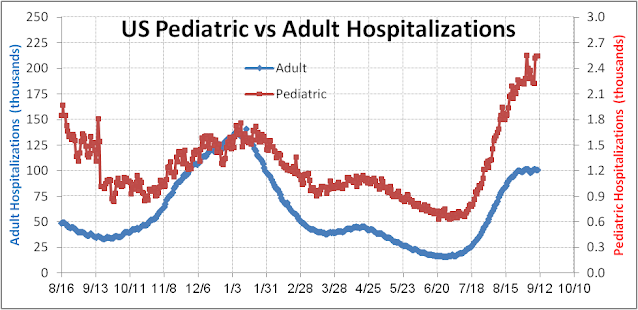
Why do we say needlessly? Because there are now proven mitigation measures that could have reduced the toll. Kids 12 and over and all staff could and should have been vaccinated. All kids and school personnel should have masked up indoors. Improved ventilation techniques such as HEPA filters could have been applied. Rapid testing could have been given to kids on a regular basis, especially those without access to vaccines. Even adopting some of these measures would have permitted in-person instruction to continue with minimal interruption. As it was, schools tried to reopen without mitigation measures and were forced to close or quarantine a large number of students – interrupting their education and producing a worse result than if they had just stayed with remote learning.
Could all this have been avoided? In California, schools reopened successfully with many of these mitigation measures in place. The difference between Texas (red curve in the figure below) and Florida (blue) with obstructionist governors, and California (green) with a governor that follows the science is striking.

Kids can return to in-person learning safely and stably. Families with elderly grandparents or immunocompromised parents can breathe easier knowing their kids are safe and they won’t be bringing home the virus. All it would take is for a governor to show true leadership and do his primary job of protecting the lives and livelihoods of his constituents.