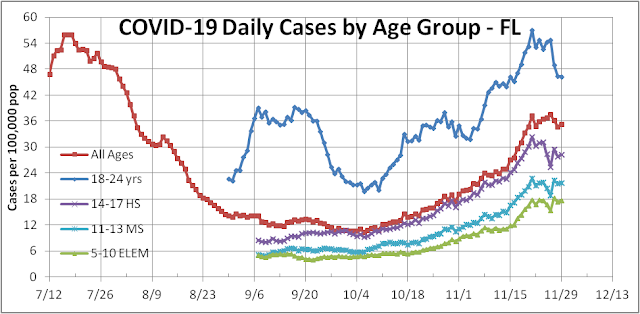
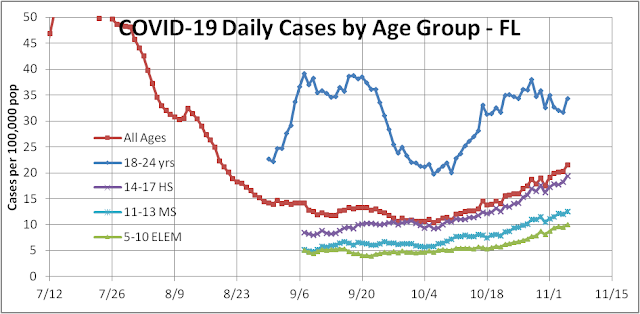
The third wave in Florida has been a little more challenging to forecast for fundamental and political reasons. The third wave in Florida began with the opening of the school year in September and began to be manifest as increased cases in early October (see figure below).
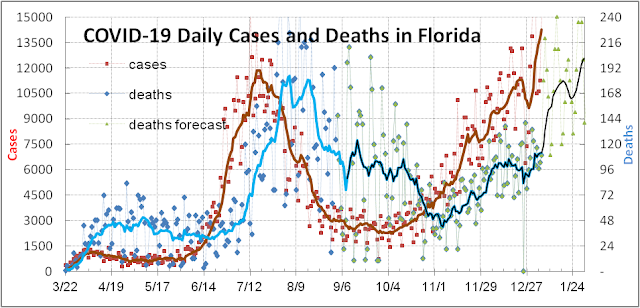
Hospitalizations began to rise two weeks later in late October (see figure below) and is now 3.66 times higher headed toward a new record.

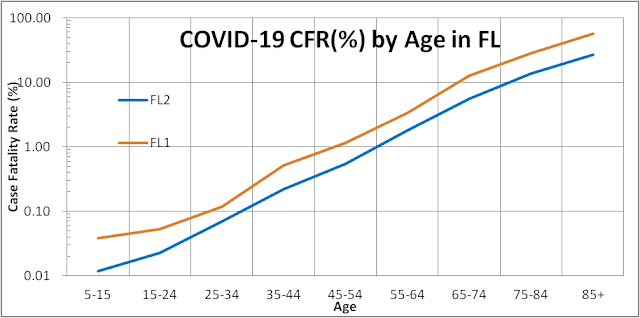
Increased deaths did not manifest itself until early November (refer back to the first figure above). All this was predictable. The less predictable part was the longer lag time or slower transmission of the virus from kids to older adults and then to grandparents who are most susceptible to fatal outcomes (see figure below).

This last transfer did not take place in large numbers until December when the weather cooled, holiday gatherings occurred, and more activities moved indoors in Florida. The mass inoculation of seniors 65+ that just began, and the rapid spread of the B.1.1.7 variant among the young should keep the median age of infectees younger in this third wave. The net effect is to lower our expectation of the case fatality rate (CFR = cases/deaths) for this third wave to 1.6% from 2.0% for the second wave.
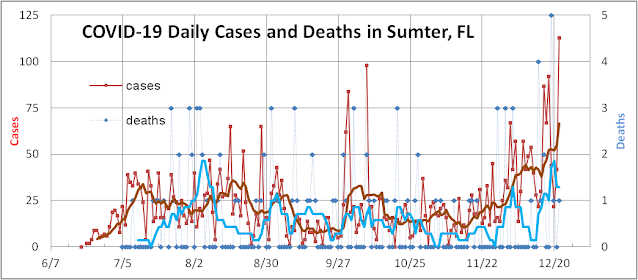
The slower than expected rise in reported death counts is also somewhat artificial due to changes in the way Florida reports deaths due to COVID-19 that stretched the COVID-19 death reporting from 2 weeks for the first wave to 2-4 weeks for the second wave to 3-8 weeks for the third wave. In the figure below, with deaths plotted against actual date, you can see that late November and December counts are still incomplete.
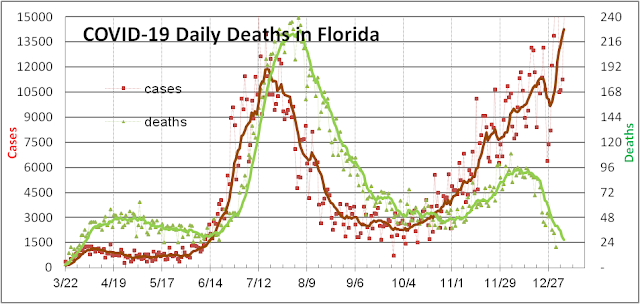
Recently some deaths from September finally got reported in January. We believe this is due to the FL Governor’s efforts to suppress reporting of deaths to make the pandemic seem less dangerous and justify his laissez-faire pandemic policies. Hopefully when the new administration takes office, there will be less motivation to politicize scientific data for the pandemic.
Our current forecast for Florida is that cases will peak in late January, hospitalizations will peak in early February and death counts will peak in late February or early March. With a combination of natural and acquired immunity (via vaccines), Florida could achieve herd immunity by summer and hopefully, avoid the fourth surge.