How does someone who gets infected by the novel coronavirus progress to symptoms to diagnosis to hospital and then to death or recovery? Much about how the virus attacks the human body remains a mystery but we can get some idea of how the typical case progresses by looking at the data that has been collected about the 18 million people that have been diagnosed with COVID-19 around the world. A significant portion of the world’s population, 100+ million, may have already been infected but never developed symptoms strong enough to warrant a diagnosis or treatment. In the USA, this number may be as high as 20 million with 4.8 million diagnosed cases. When a person is diagnosed, it may take 3-12 days before symptoms develop if they develop at all. When they do develop symptoms they may ask for a test which can take a few days to return with a result. If positive they may be asked to quarantine in place at home for 14 days or be admitted to a hospital if the symptoms are severe enough. The latter are treated in a hospital and if severe enough may progress to ICU and ventilator. All along this journey some may recover and be discharged from the pool of active patients or they may die. In the USA, 157 thousand have died while 2.4 million have recovered. The census of recoveries is clearly undercounted since the number of known active cases in the USA is probably less than 1 million. The more information we have about the structure of this pipeline the better we can model and forecast the progression of this disease and subsequent outbreaks.
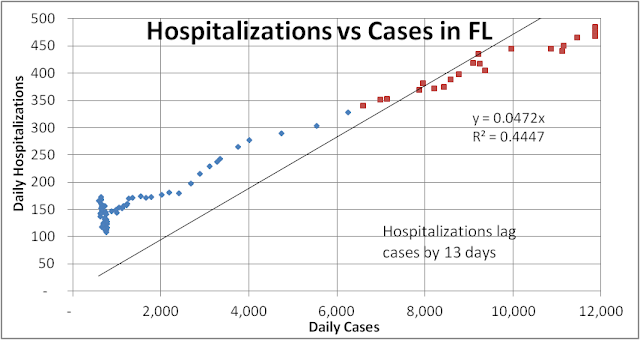
Once a case is identified we can begin to track its progress through the pipeline. Single-day counts have a lot of noise and are dominated by the 7-day weekly cycle so we use 7-day rolling averages for all the Florida (FL) data analyzed below. The figure below shows the correlation between hospitalizations and cases identified 13 days earlier. Most patients are tested and sent home to quarantine and wait for test results. If and when their symptoms worsen they are then hospitalized with an average lag time of 13 days. As many as 25% (=150/600) of the early cases led to hospitalizations when testing was limited to the most severe cases (the cluster at the lower left). As testing widened a decreasing percentage went to hospitalization in July (brown squares at the upper right) and fell below the average hospitalization rate of 4.7% represented by the best-fit slope.
Most of the confirmed COVID-19 deaths occur in hospitals so we would expect deaths to correlate well with hospitalizations with a lag. The best-fit lag is 6 days. The best-fit slope indicates that 30% of all Floridians who require hospitalization will ultimately die. This lag time and correlation have not changed much from spring to summer so there seems to be little improvement in therapeutics to improve outcomes. In fact, July data shows that when the hospitalization rate got high and facilities and resources in counties such as Miami-Dade may have been stretched, death rates increased above trend.

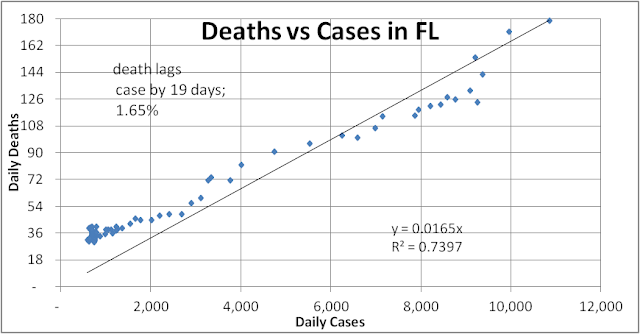
Deaths also correlate with cases. Deaths lag case diagnosis by 19 days. This is now much longer than the average of 9 days that were typically seen at the early stage of infection when tests were only given to those with serious symptoms or who were most likely infected. With more testing, mild and asymptomatic cases are now identified and symptomatic cases are identified earlier before they need to go to hospitals. The best-fit slope is the case fatality rate (CFR=deaths/cases) of 1.65%, much better than the roughly 6% (36/600 = cluster of data at the lower left above the trend line) seen at the beginning of the spring outbreak in FL.
Given this strong correlation, we can then use the daily case counts to forecast the daily death counts that are sure to follow 19 days later. If we had good age, gender, and comorbidities data we could refine our prediction for the number of patients that will need hospitalization 13 days after diagnosis and the death rate to follow 6 days later. This is how we forecast the death count over the next 3 weeks for the USA and every state and county in the USA.

The case counts in Florida peaked on 7/17 and we would expect the death count to peak on 8/4. A plot of new daily hospitalizations peaked on 7/30 and confirms the 8/4 date for the death count peak.

This is good news for Florida and some of the other Sunbelt states such as Texas, California, and Arizona, but because these peak rates are very high there is little reason to celebrate yet. In fact, given that some schools are reopening around the country this month at the urging of the President, we need to remain ever vigilant to avoid a fall resurgence of the spring and summer surges. A fall resurgence could be more problematic as it will overlap with seasonal flu cases that usually begin in October.

Leave a Reply